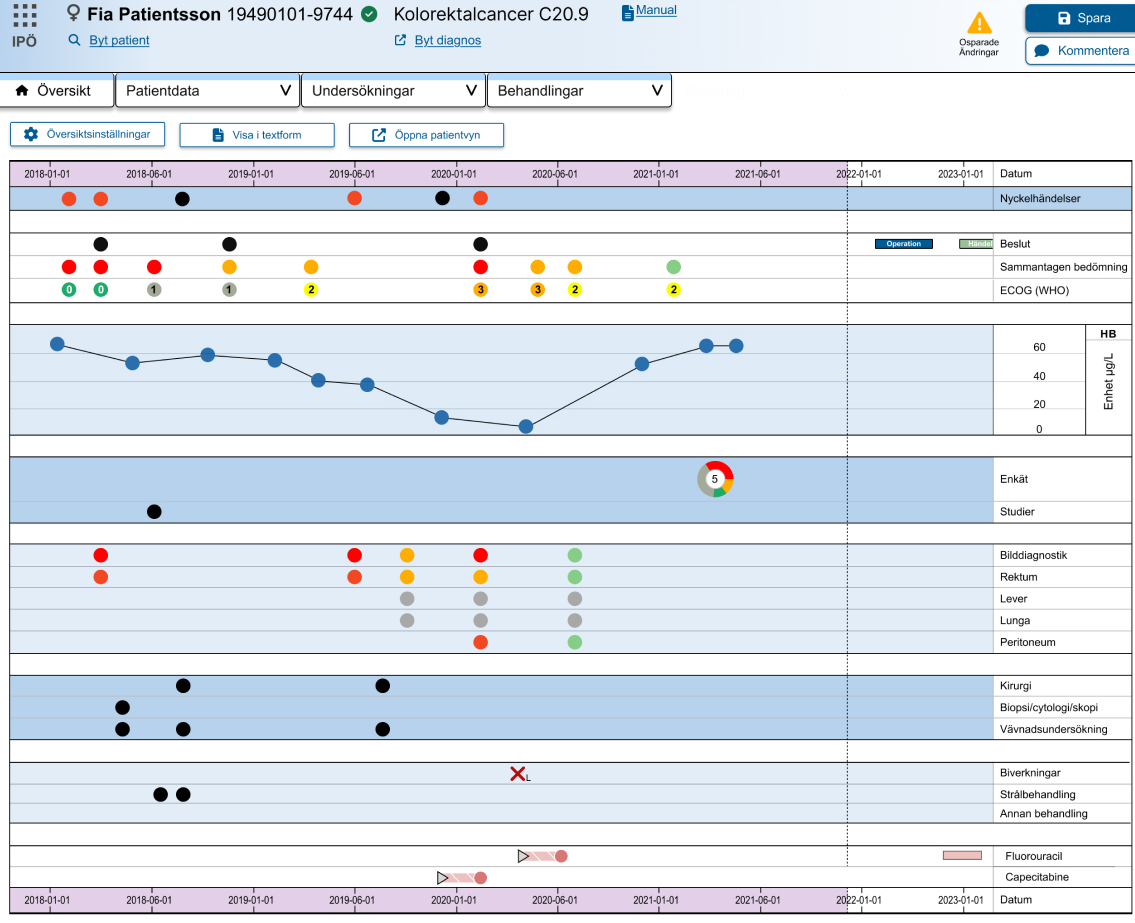
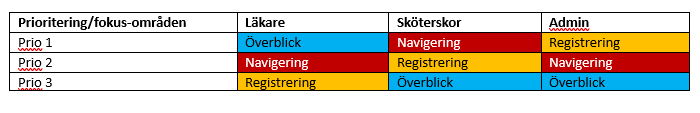
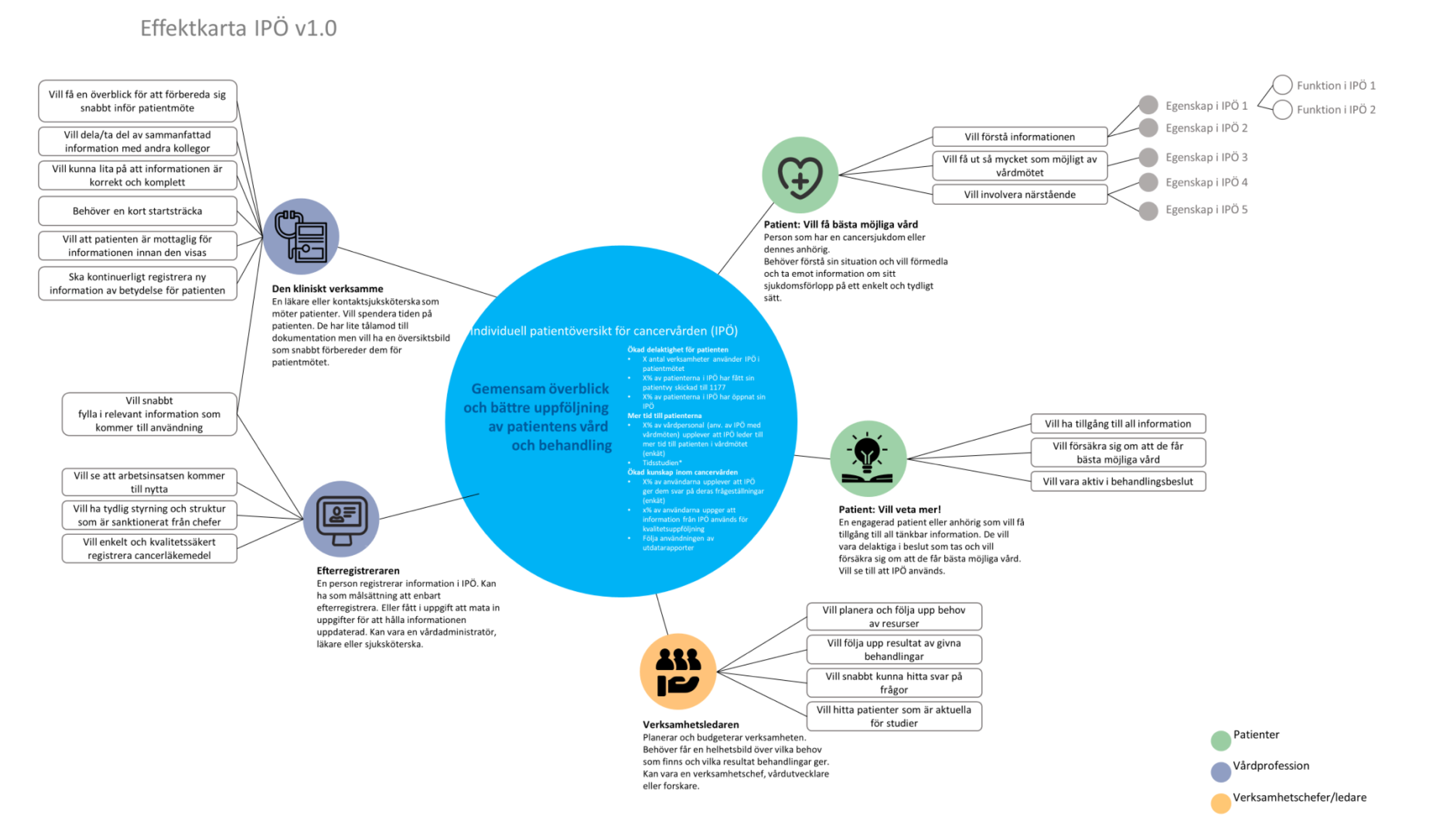
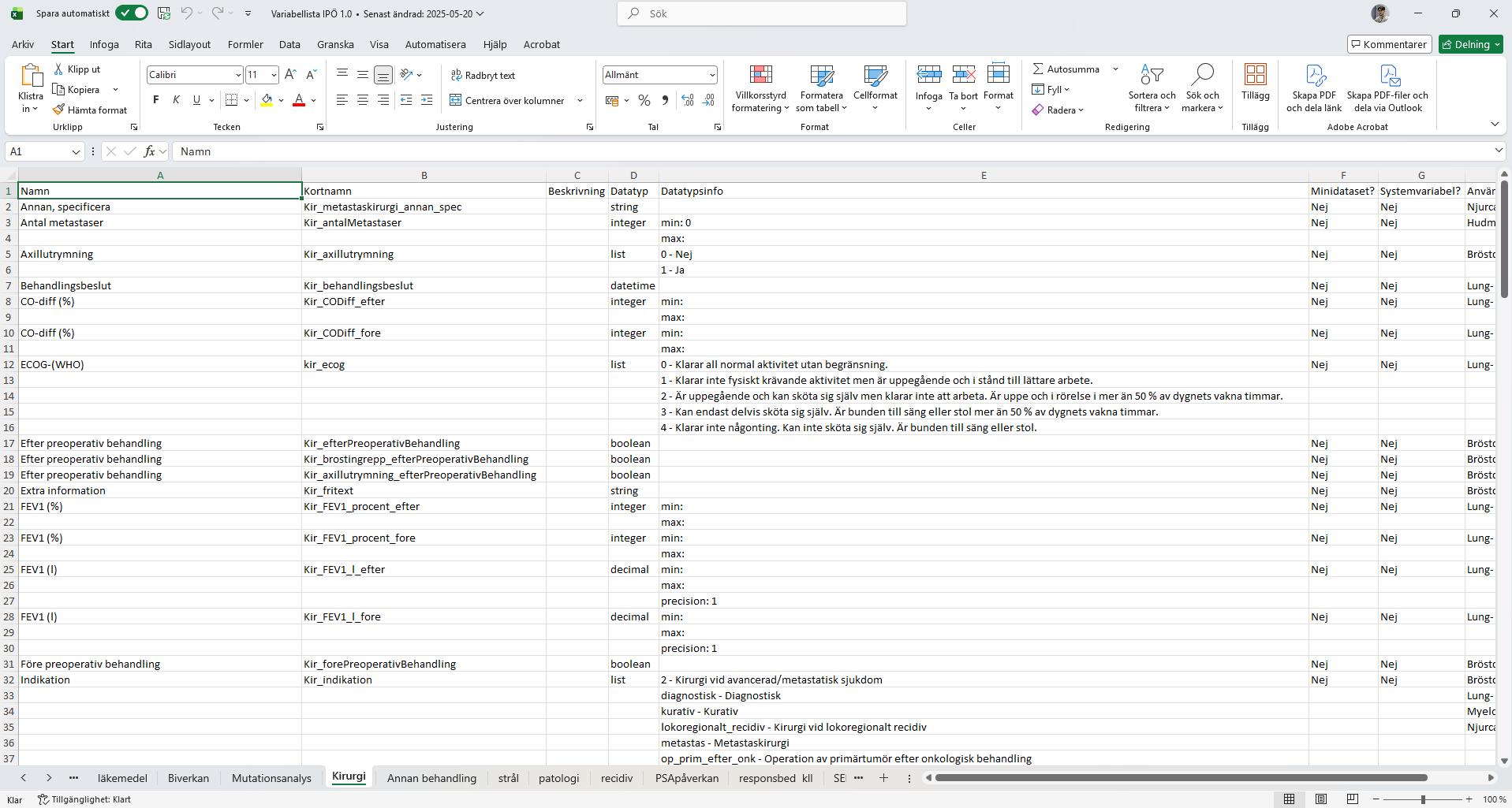
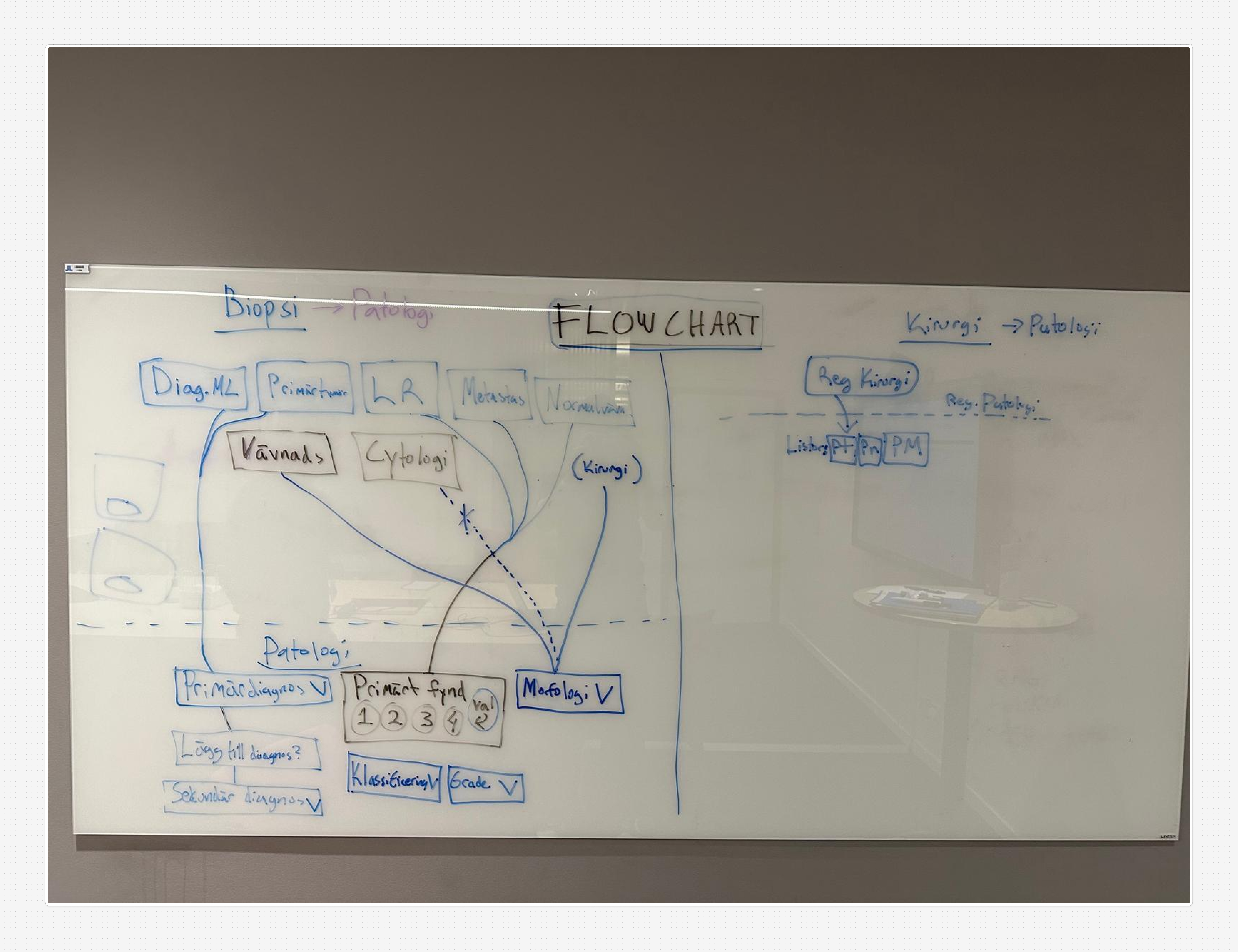
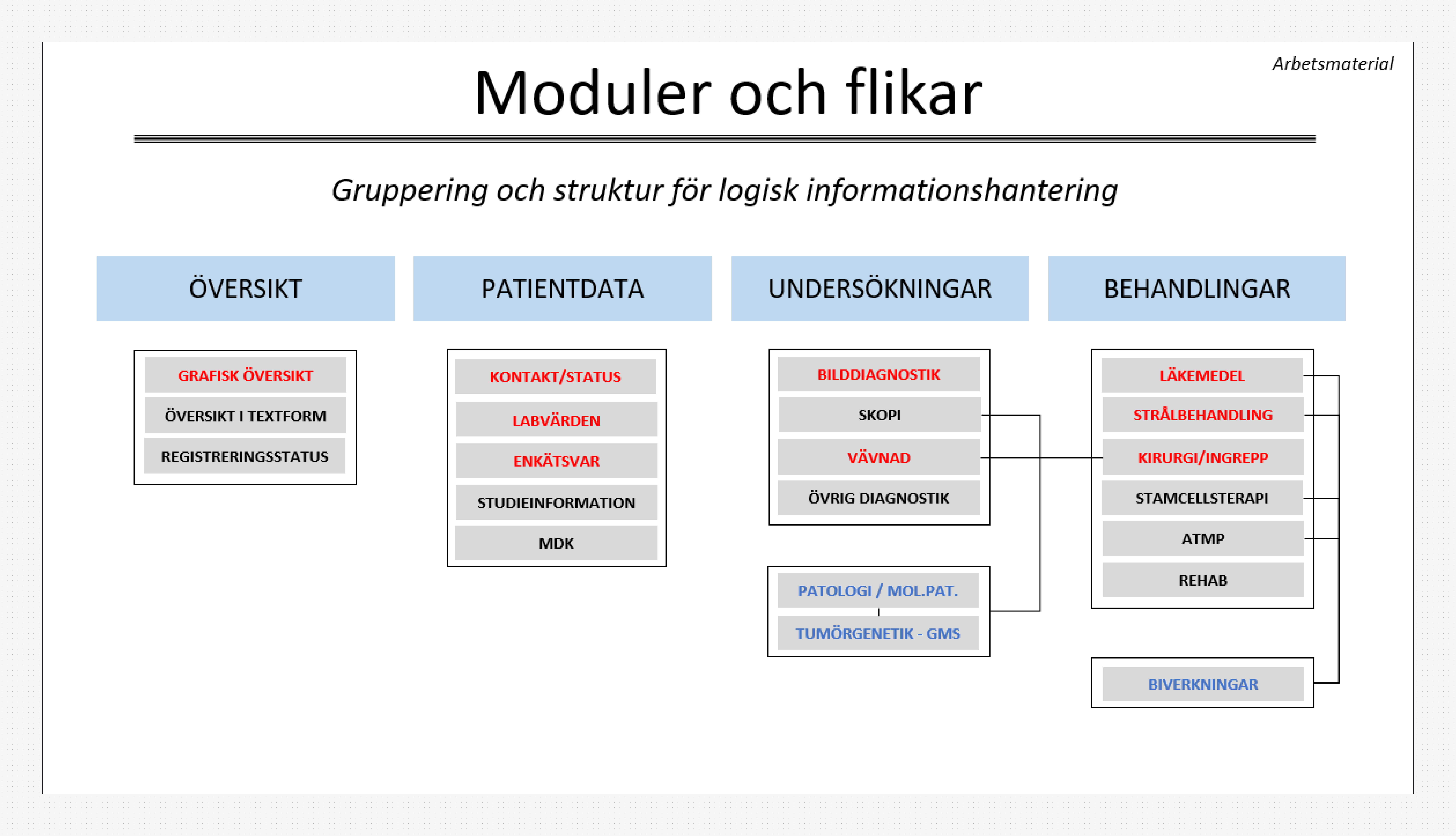
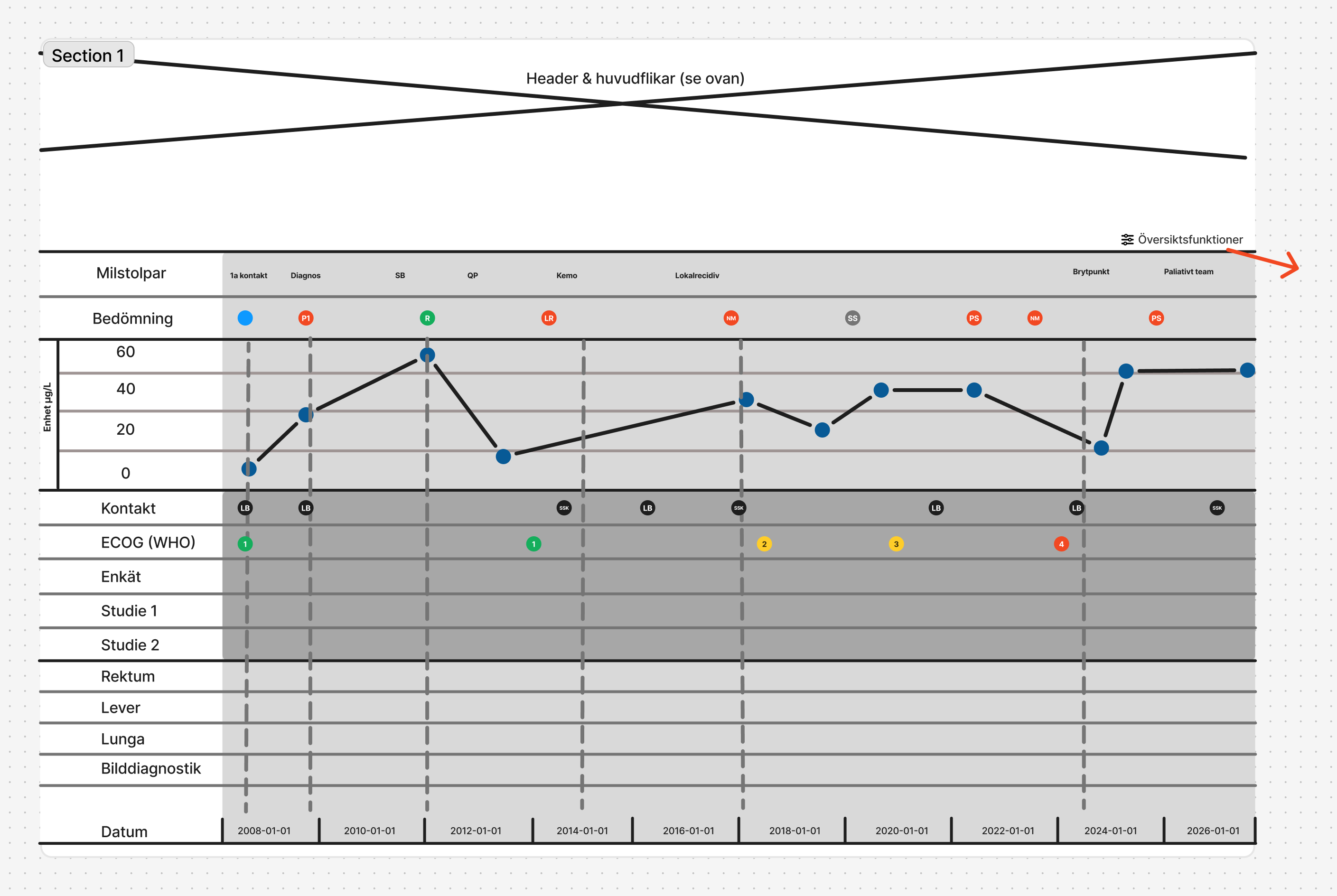
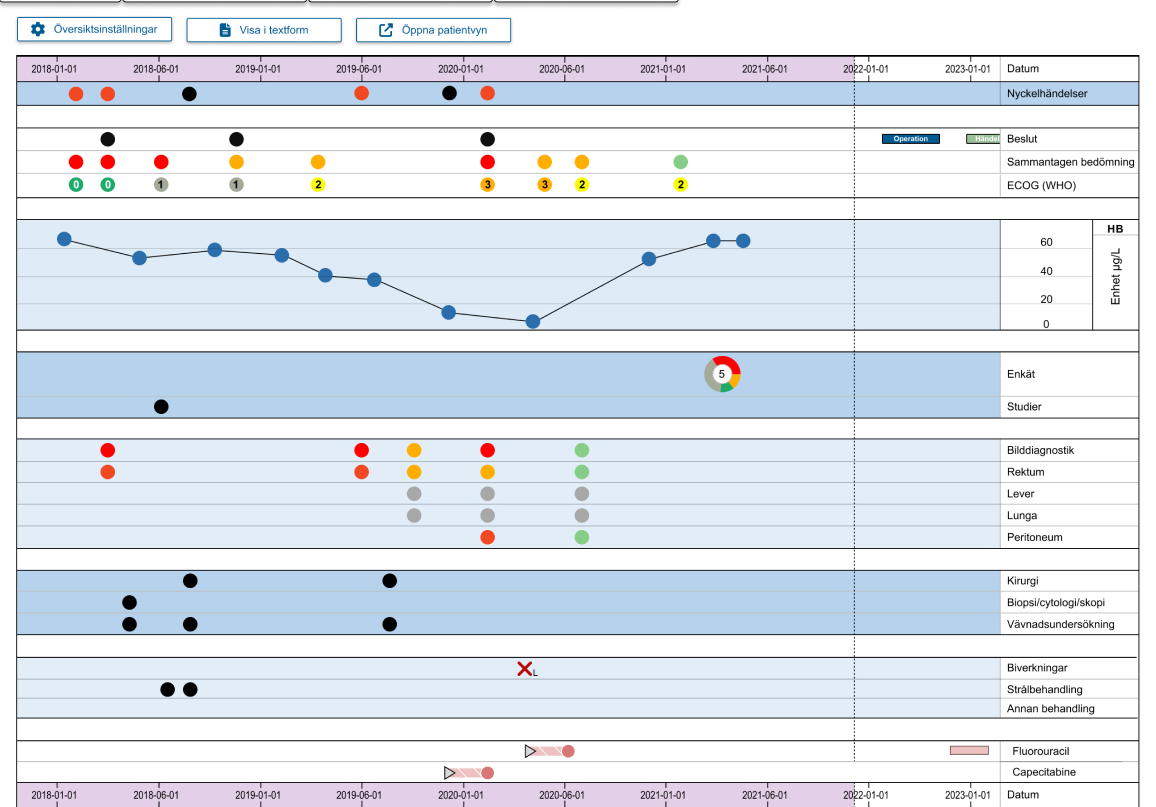
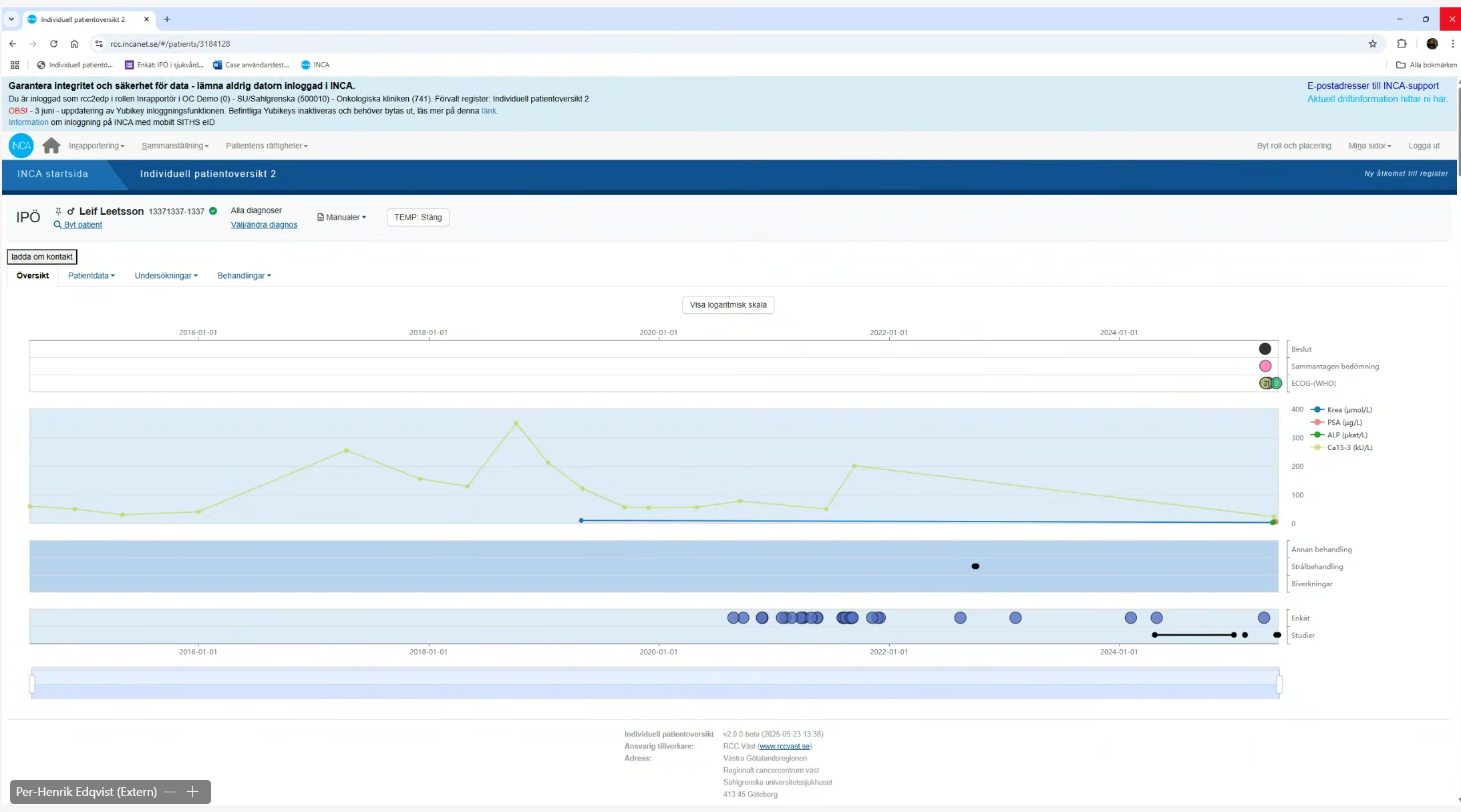
This project demanded a methodology that could handle two distinct layers of complexity simultaneously: the human layer (three professional roles with genuinely different needs) and the technical layer (a variable-driven backend that had to be fully understood before a single screen could be designed).
Rather than moving straight to wireframes, the process started with alignment and comprehension. Every design decision that followed was traceable back to either a user need, a flow, or a variable in the underlying data structure.